EARLY GOAL-DIRECTED THERAPY IN THE TREATMENT OF SEVERE SEPSIS AND SEPTIC SHOCK
E MANUEL R IVERS , M.D., M.P.H., B RYANT N GUYEN , M.D., S UZANNE H AVSTAD , M.A., J ULIE R ESSLER , B.S.,
A LEXANDRIA M UZZIN , B.S., B ERNHARD K NOBLICH , M.D., E DWARD P ETERSON , P H .D., AND M ICHAEL T OMLANOVICH , M.D.,
NEJM 2001
The purpose of this study, often referred to as the Rivers trial, was to evaluate the efficacy of early goal directed therapy before admission to the intensive care unit.
A prospective, randomised study.
Inclusion criteria :
Fulfillment of two of the four SIRS criteria and…
Systolic blood pressure less than or equal to 90mmHg (after a fluid challenge of 20-30ml/kg over a 30 minute period) or….
Lactate greater than or equal to 4 mmol/litre
Exclusion criteria :
Aged less than 18 years
Pregnancy
Or presence of an acute cerebral vascular event, acute coronary syndrome, acute pulmonary edema, status asthmaticus, cardiac dysrhythmias (as a primary diagnosis), contraindication to central venous catheterization, active gastrointestinal hemorrhage, seizure, drug overdose, burn injury, trauma, a requirement for immediate surgery, uncured cancer (during chemotherapy), immunosuppression (because of organ transplantation or systemic disease), do-not-resuscitate status, or advanced directives restricting implementation of the protocol.
Method
Two groups.
One treated with clinician lead standard therapy after arterial and central venous catheterisation. Blood and cultures taken before administration of antibiotics which were given at the discretion of the clinician.
Other group assigned to early goal directed therapy (EGDT). Insertion of arterial line and central venous catheter capable of measuring central venous oxygen saturations. Treated in the emergency department by the clinicians for at least six hours. Protocol as follows:
- 500 ml bolus every 30 mins to achieve CVP 8-12 mm Hg
- If MAP < 65 mm Hg give vasopressors
- If MAP > 90 mm Hg give vasodilators
- If central venous sats < 70% give red cells to achieve heamatocrit of at least 30%
- Dobutamine if above optimised and central venous sats still < 70%
Primary endpoint – In hospital mortality.
Secondary endpoint – resuscitation end points, organ-dysfunction scores, coagulation-related variables, administered treatments, and the consumption of health care resources.
Main results.
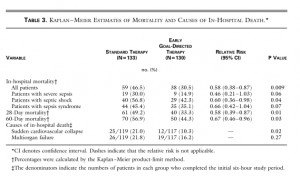
In hospital mortality rates significantly higher in standard therapy group (46.5%) compared to EGDT group (30.5%).
28 day mortality significantly higher in standard therapy group (49.2%) compared to EGDT group (33.3%).
60 day mortality significantly higher in standard therapy group (66.9%) compared to EGDT group (44.3%).
During initial six hours patients in EGDT received significantly more fluid (4.9l +/- 2.9l) compared to standard therapy (3.4l +/- 2.4l) and more frequently received red blood cells and inotropic support. However after 72 hours there was no difference. So the EGDT group got their fluid faster than the standard therapy group.
Hospital length of stay significantly different in standard therapy (18.4 +/- 15) compared with EGDT (14.6 +/- 14.5)
Study weaknesses/criticisms
Only one centre involved. A higher level study would have been a multi-centre trial.
Use of Edwards Life Science catheter which has significant cost – do we really need continuous monitoring or can we take regular samples instead?
The population in this study seem far sicker than any recruited in studies done since. Was there some bias with the sample of patients in the Detroit area where this study was done? See article in Chest.
Overall this piece of research probably meant that patients were treated more aggressively with fluids than before the article was published and that there is an increased emphasis on moving the patients to the ITU as quickly as possible.
Links to others viewpoints
See Jones Trial- Is Lactate Clearance a Useful Indicator on this website
EMBasic- Introducing EM Basic Essential Evidence- The Rivers Sepsis Study
Paul Mariks assertion that Lactate clearance is flawed
EMCRIT- Podcast 54- Dr Rivers on Severe Sepsis
[Stitcher_Radio_Logo]
[get_in_touch_with_jonathan]
[123-contact-form i882618]