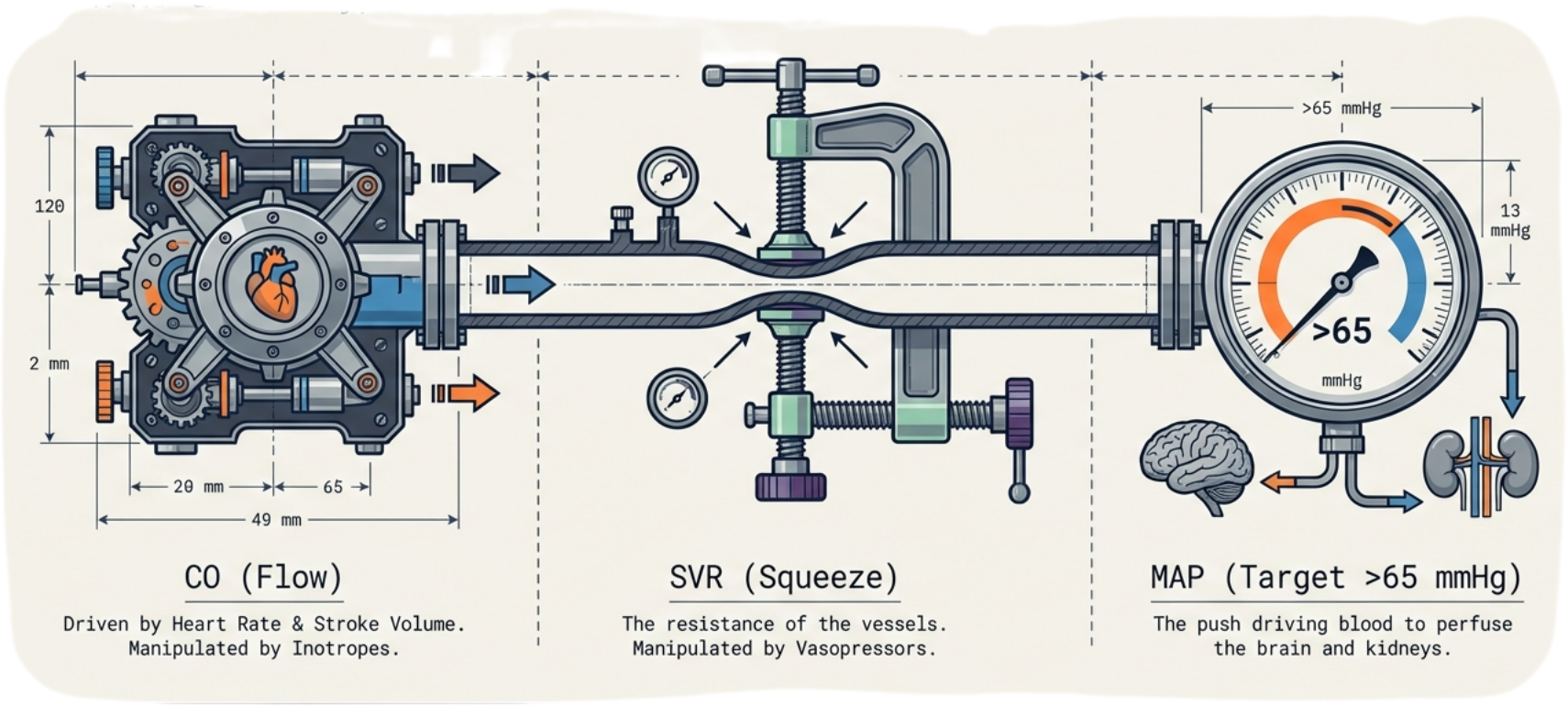
Shock is fundamentally defined as tissue hypoxia, where a supply-demand mismatch prevents organs from meeting metabolic needs. To restore stability, clinicians manipulate the equation MAP = CO × SVR, targeting a Mean Arterial Pressure (MAP) of 65 mmHg to maintain vital organ perfusion
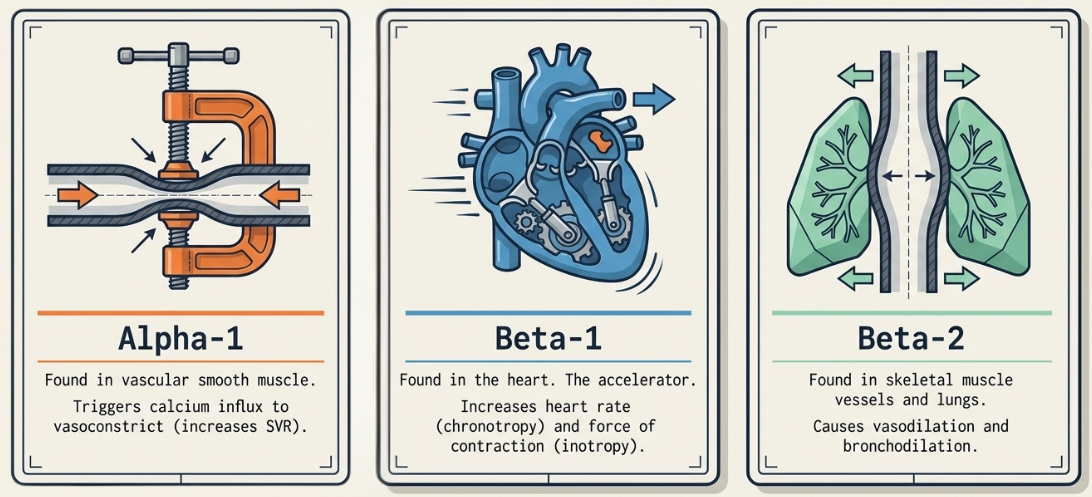
The Adrenergic Workhorses
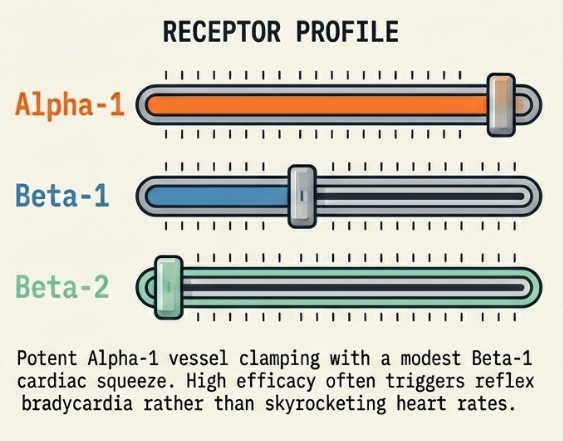
- Noradrenaline (Norepinephrine): The first-line agent for almost all shock states, particularly septic shock. It is a potent α1 agonist that increases Systemic Vascular Resistance (SVR) while providing modest β1 support for cardiac contractility. Dosing typically ranges from 0.01 to 0.4 mcg/kg/min.
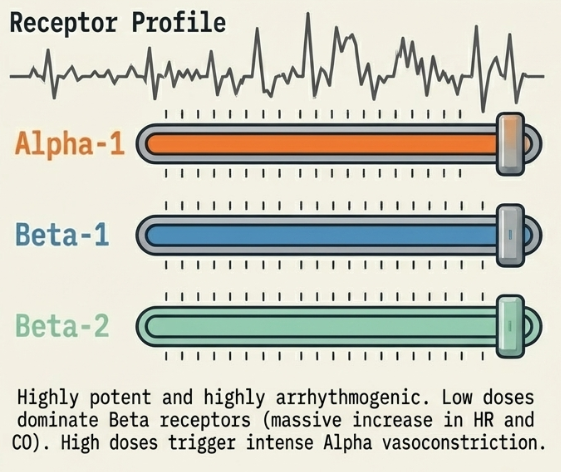
- Adrenaline (Epinephrine): A potent, non-selective agent hitting α and β receptors. Low doses primarily increase cardiac output (CO) via β effects, while high doses cause intense vasoconstriction. It is highly arrhythmogenic and can trigger the "lactate trap," where stimulated glycolysis raises serum lactate even if perfusion is improving.
Noradrenaline
Adrenaline
Inotropes and Temporary Support
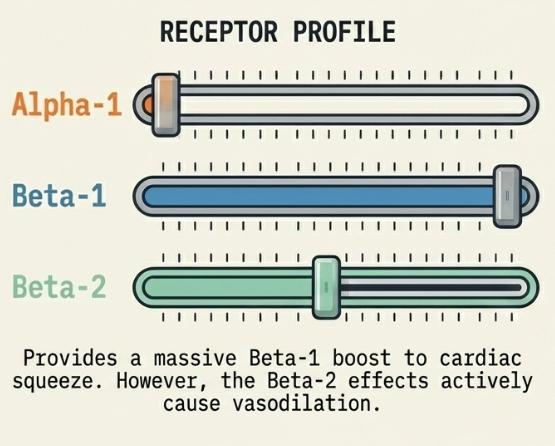
- Dobutamine: A synthetic inodilator acting on β1 and β2 receptors. It increases contractility and CO but may cause vasodilation and hypotension, necessitating combination with a pressor. Standard dosing is 2–20 mcg/kg/min.
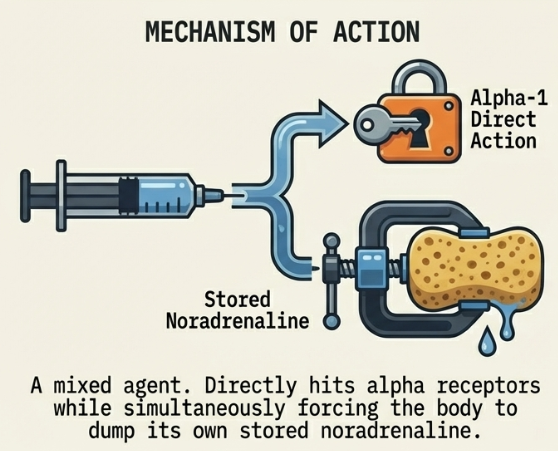
- Metaraminol: A mixed direct/indirect agent that triggers the release of stored noradrenaline. Used for short-term hypotension, it carries a high risk of tachyphylaxis, becoming ineffective once the body’s noradrenaline stores are depleted.
Dobutamine
Metaraminol
The Non-Adrenergic Secret Weapon
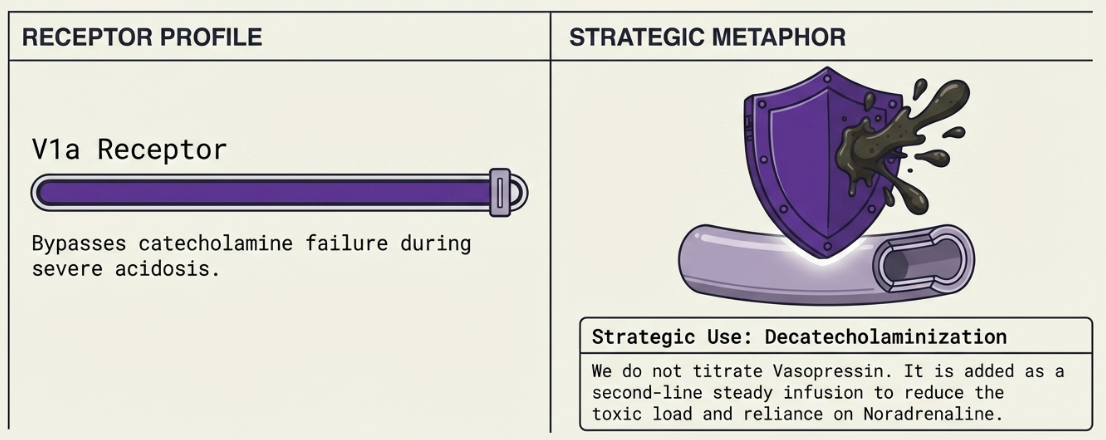
- Vasopressin: Acting on V1a receptors, it provides vasoconstriction through a pathway independent of catecholamines. It remains effective during acidosis, where other drugs often fail. It is primarily used for "decatecholaminization"—adding it as a second-line adjunct to lower toxic noradrenaline requirements, which helps protect renal function and reduce arrhythmias. It is typically given at a fixed dose of 0.03 units/min.
Critical Care Implications
- Vascular Access: Ideally, these drugs are vesicants and must be infused through a central line to prevent tissue damage. Peripheral administration is a temporary bridge; if used, clinicians should select a large vein proximal to the antecubital fossa and limit duration.
- Extravasation Management: If a peripheral line leaks into the tissue, it is a medical emergency. Immediate steps include stopping the infusion, aspirating the drug, and administering the antidote Phentolamine. Evidence-based alternatives during shortages include topical nitroglycerin or subcutaneous terbutaline.
- Monitoring: Continuous blood pressure monitoring via arterial line is essential for accurate titration and clinical assessment of perfusion markers like mentation and urine output
