Respiratory System- Anatomy
The respiratory system goes from the nose and mouth all the way to the alveoli. However it does not stop there when trying to understand the way we breath, taking in oxygen and eliminating waste gases.
We also need to understand respiration at a cellular level to gain some understanding of how various conditions can cause ill health.
The Nose
Anatomy
There is an internal and an external part to the nose. The bridge of the nose is composed of bone which supports the hyaline cartilage which is covered by muscle and skin and lined by the mucous membrane. The openings on the underside are called the nostrils or nares.
Internally the cavity of the nose lies below the cranium and above the roof of the mouth. It communicates at the back with the pharynx.

Ducts from the paranasal sinuses and the nasolacrimal ducts also open into the internal nose.
The inside of the nose is divided into right and left sides by the nasal septum.
The front part of this is made from cartilage
Physiology
The interior of the nose serves 3 functions:
- warms, moistens and filters the incoming air.
- smell.
- chambers modify speech sounds.
The vestibule at the front of the nose is lined with hairs that filter out large dust particles. Three shelves, the conchae, project out form the lateral walls to almost touch the septum.
These then subdivide into a series of groove like passageways- the superior, middle and inferior meatuses.
This is lined with mucus membranes, and the olfactory receptors are in the epithelium lining the superior nasal conchae.
The mucus membrane contains capillaries and epithelial cells with many goblet cells. Air is warmed by the blood in the capillaries and dust is trapped by the mucus secreted by the goblet cells. The cilia within the nose moves the dust/mucus to the pharynx so they either be swallowed or expelled.
Pharynx
The pharynx is divided into the nasopharynx and the oropharynx and laryngopharynx.
The nasopharynx is the uppermost portion and extends from the internal nares to the level of the soft palate. There are openings to the Eustachian tubes and the posterior walls have the pharyngeal tonsil, or adenoids. Cilia move dust particles down and there is an exchange of air via the Eustachian tubes to equalise the pressure in the ears, nose and throat.
The oropharynx extends from the level of the soft palate to the level of the hyoid bone. It is a common passageway for both air, food and fluid. The palatine and lingual tonsils can be found here.
The laryngopharynx extends from the hyoid bone and joins with the oesophagus at the back and the trachea at the front.
Larynx
The wall of the larynx is comprised of:
- Three single cartilages- thyroid, epiglottis and cricoid.
- Three paired cartilages- arytenoid, corniculate and cuneiform.
The thyroid cartilage is composed of two fused plates of hyaline cartilage and is bigger in males than females.
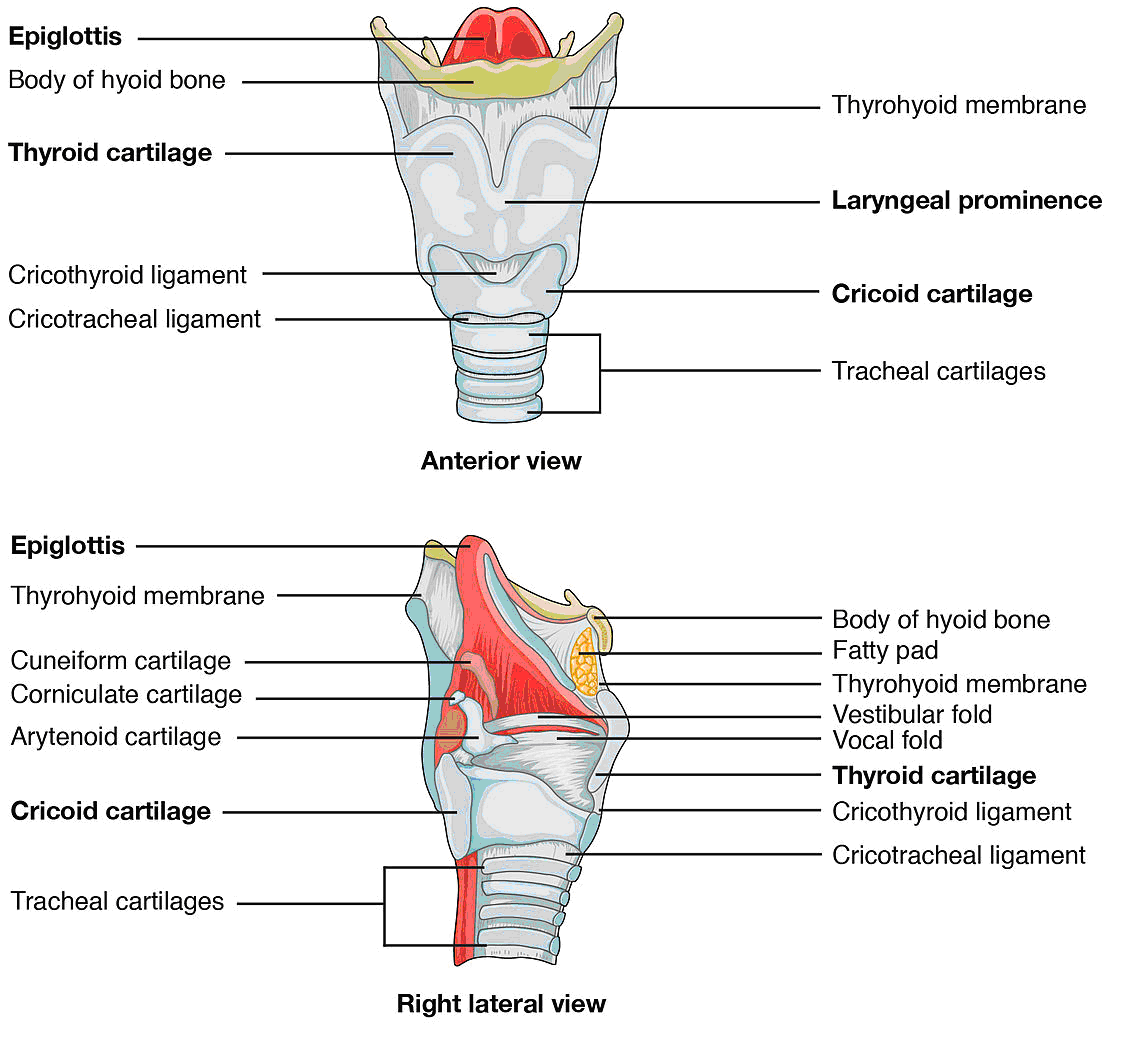
The epiglottis is leaf shaped and has its stem attached to the anterior rim of the thyroid.
The larynx elevates during swallowing and the free top edge of the epiglottis covers the glottis. This prevents foreign bodies, food or liquid entering the trachea.
The cricoid is a ring of hyaline cartilage attached to the first ring of cartilage of the trachea.
The paired arytenoid cartilages are triangular pieces of mainly hyaline cartilage and they attach to the vocal folds and intrinsic pharyngeal muscles and they move the vocal folds.
The lining of the larynx below the vocal folds consists of ciliated and goblet cells and the mucus traps dust with the cilia moving the trapped particles upwards.
There are two pairs of folds in the larynx mucous membrane.
The upper pair are called the ventricular folds (false vocal cords) and a lower pair called the vocal folds (true vocal cords).
Elastic ligaments within the folds are pulled by muscles of the larynx which can then stretch the vocal folds so that the opening, or glottis, is narrowed. As air is directed to these folds vibrations are set up.
Pitch is controlled by the tension on these vocal folds and, along with the shape of the pharynx, mouth , nasal cavity and paranasal sinuses, sound can be made and hence speech.
Trachea

The trachea extends from the larynx to the fifth thoracic vertebrae, and lies in front of the oesophagus. At its lower end it divides into the left and right main bronchus.
The wall of the trachea consists of the mucosa, submucosa, hyaline cartilage and adventitia. The epithelium of the mucosa consists of ciliated columnar cells and goblet cells, which provide the same protection against dust as the membrane lining the larynx.
The rings of cartilage around the trachea are C shaped with the open side against the oesophagus, which allows the oesophagus to expand slightly during swallowing.
The C shaped cartilage provide support so that the trachea does not collapse inwards.
Where the trachea divides left and right, there is an internal ridge of cartilage called the carina. This area is very sensitive and is associated with the cough reflex.
Bronchi

The trachea divides into the left and right primary bronchus. Like the trachea these contain incomplete rings of cartilage.
Once in the lung these bronchi then divide into the secondary or lobar bronchi which then further divide into the tertiary or segmental bronchi
Then there is division into the bronchioles which branch into ever smaller bronchioles and eventually into terminal bronchioles.
As the branching develops several changes take place:
- epithelium changes from ciliated to non ciliated. Inhaled particles lower down the bronchial tree are dealt with by macrophages.
- Incomplete rings of cartilage are replaced by plates of cartilage which also disappear in the terminal bronchioles.
- The amount of smooth muscle increases, encircling the lumen in spiral bands.
Lungs

There are two serous membranes which surround the lung, called the pleural membrane.
The outer layer, the pleural membrane, is attached to the thoracic cavity and the inner layer, the visceral membrane, covers the lungs themselves.
Between these layers is the pleural cavity, which is a potential space containing a lubricating fluid to allow the membranes to move easily against each other.
Gross Anatomy

The lungs extend from just above the clavicles down to the diaphragm, and they lie against the ribs front and back.
The bottom part of the lung is often referred to as the base and the upper part as the apex.
The surface of the lung lying against the ribs is called the costal surface, and the surface of each lung facing the heart, or medial side (in the mid line) contains the hilus through which pass bronchi, pulmonary blood vessels, lymphatic vessels and nerves.
The left lung also has a notch which provides room for the heart, known as the cardiac notch.
The right lung is divided into three lobes, upper, middle and lower and the left lung into two, upper and lower.

Between these lobes are the fissures. Each lung has an oblique fissure extending downwards and forwards. The right lung also has a horizontal fissure, reflecting the fact that it has one more lobe than the left.
As we move towards the segments of the lungs, the division after the lobes, we encounter the lobules. Each one contains a lymphatic vessel, an arteriole, a venule and a branch from a terminal bronchiole. The terminal bronchiole subdivides into respiratory bronchioles which then further sub divide into alveolar ducts.
Around the alveolar ducts are alveoli and alveolar sacs. The alveolus is lined by epithelium and contains two types of cells, type I and type II.
Type II alveolar cells secrete, amongst other things, surfactant which reduces the surface tension thereby making it easier to keep the alveoli open.
There are also macrophages within the alveolar wall whose job is to remove dust particles or other debris from the alveolar
Blood supply to the lungs
Deoxygenated blood passes from the heart via the pulmonary trunk which divides into the left and right pulmonary artery which enter the respective lungs.
The oxygenated blood is returned via the pulmonary veins, two on each side , the superior and inferior pulmonary veins. All four of these vessels drain into the left atrium.
The resistance in the pulmonary system is lower than in the systemic circulation. Pulmonary vessels will also constrict where there is hypoxia whereas in the systemic circulation, vasodilatation will occur in similar circumstances.
Guidelines for the management of tracheal intubation in critically ill adults
Having read the guidelines I made these infographics. They are FREE. Just click on the button below.





